Dr Punam on BBC Morning Live recommends Acupuncture as part of the strategy for Fibromyalgia symptoms
Here are the links to the original show: BBC Morning Live Series 6: 13/06/2024 (from 20 to 28 minutes, approximately). Link to the specific 8-minute segment: BBC One – Morning Live, What is fibromyalgia syndrome?
Understanding Fibromyalgia: Unravelling the Mystery
Recently, on Morning Live (BBC), Dr Punam shed light on fibromyalgia—a chronic condition that affects countless lives. The show’s presenters emphasized its prevalence, with viewers flooding their social media channels to share their experiences. Among the poignant messages were:
Amanda – “Professionals have told me it’s in my head or it’s not a real illness! I lost my job I loved. I almost lost my home”
Linda – “No-one believes how much pain you can be in. it can make you feel down and useless sometimes”
Sharon – “It is an awful condition in constant pain but because it’s invisible most people don’t understand”
What is Fibromyalgia?

Dr. Punam explained that fibromyalgia manifests in various ways: widespread pain, extreme fatigue, and cognitive challenges (commonly referred to as “fibro fog”). Despite affecting approximately one in 20 people, the condition remains enigmatic.
The underlying mechanism involves altered pain processing in the spinal cord and brain. These individuals have elevated levels of certain pain-signalling chemicals, rendering them hypersensitive to pain. Dr Punam said “I have patients regularly they’re dealing with shooting pains feeling electric shocks […] you can really imagine having to live with that every day”
Fibromyalgia can run in families and most commonly impacts people between the ages 25 and 55, but cases have even been seen in children. Triggers include trauma (like car accidents), major life events (such as bereavement), post-viral illnesses, and even childbirth. Yet, we lack a comprehensive understanding of why it occurs.
The Stigma and Struggle
Sadly, fibromyalgia sufferers face stigma due to widespread ignorance. Many feel unheard, their symptoms dismissed. As a GP, Dr Punam shared that she empathised deeply because her own mother has battled fibromyalgia for decades, and she spoke of her mother’s transformation from an active woman to one crippled by fatigue and pain. Doctors had dismissed her when tests came back clear, with one claiming “it’s all in your head.”
“When you have instances like this, the person that’s affected will feel like they are unsupported, it increases isolation, it can even lead to depression” Dr Punam says, “I think it adds to the general lack of empathy we have in society towards invisible conditions, not just fibromyalgia, chronic fatigue syndrome, autoimmune conditions.” Progress is being made, but there’s still a long road ahead, she reflects.
The symptoms disrupt lives—people who once held jobs, managed households, and cared for children now feel like shadows of themselves. Diagnosis remains challenging; it’s exclusionary, relying on detailed history, clinical exams, and negative test results.
Understanding Fibromyalgia Symptoms
Familiarising ourselves with fibromyalgia symptoms is crucial. Here’s a concise list:
- Pain sensitivity
- Muscle Stiffness
- Fatigue
- “Fiibro-Fog”
- Irritable bowel syndrome
Pain Sensitivity and Muscle Stiffness:
Fibromyalgia isn’t localized pain; it can affect any part of the body: Individuals become hypersensitive to even the lightest touch.
Fatigue:
This is not a generalised tiredness, it’s a depletion of energy and extreme fatigue. “This is like waking up after hours of sleep and still feeling exhausted” says Dr Punam, and overexertion exacerbates the draining effect.
“Fibro-Fog”:
- This cognitive challenge affects memory and concentration.
- In the workplace, lack of support can make it particularly difficult.
Gut Issues:
- Irritable bowel syndrome (IBS) is common in fibromyalgia.
In addition to the above, restless leg syndrome and headaches may also occur.
Managing Fibromyalgia: Strategies and Support
According to Dr Punam, while there’s no cure, several approaches can alleviate symptoms and flare-ups:
- Heat:
- Heat helps with stiff joints.
- Try warm baths, hot water bottles, or soaking hands and feet in warm water.
- Pain Relief:
- Painkillers, both over-the-counter and prescription, can provide relief.
- Exercise:
- Proceed with caution; work within your abilities.
- Exercise benefits mood, releases endorphins, and improves symptoms.
- Consult your GP for a referral to specialised exercise guidance.
- Talking Therapies:
- Cognitive-behavioural therapy (CBT) helps manage thought processes.
- Address issues arising from flare-ups.
- Complementary and Integrated Approaches:
- Acupuncture has shown promise.
- Yoga and Tai Chi can be beneficial.
- Individualized Management:
- What works varies from person to person.
- Support from healthcare professionals, family, friends, and colleagues is essential.
- Antidepressants:
- Beyond mood improvement, certain types can manage pain and enhance sleep quality.
Remember, you’re not alone in this journey. Seek support and tailor your management plan to your unique needs.
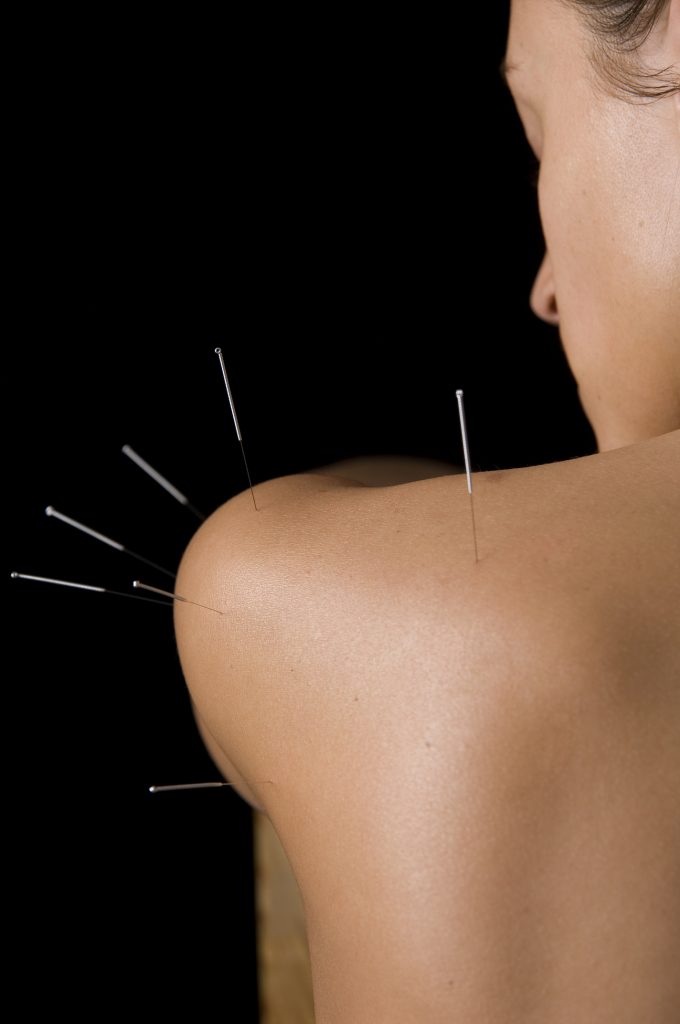
Acupuncture with Shaftesbury Clinic
Adding to the above, where Dr Punam mentioned studies for acupuncture, we have a dedicated page for information and research: Shaftesburyclinic.com Fibromyalgia: Condition Resources which may be of interest.
Acupuncture can be a part of your approach to coping with the symptoms of fibromyalgia, and it is always good to have an overall approach that takes into account your individual needs and symptoms. You should always go in the first instance to your GP or pain consultant, but we are very happy to liaise with them about your care, and we often receive referrals from medical colleagues for chronic pain.
Also good to note, is that the NHS advisory panel, NICE (National Institute for Health and Care Excellence), have recommended acupuncture for chronic pain, as per our blog about this subject here: Shaftesburyclinic.com: acupuncture and chronic primary pain – the new nice draft guidelines
Links
https://www.bbc.co.uk/iplayer/episode/m00202kr/morning-live-series-6-13062024
https://www.bbc.co.uk/programmes/p0j3yvgz


