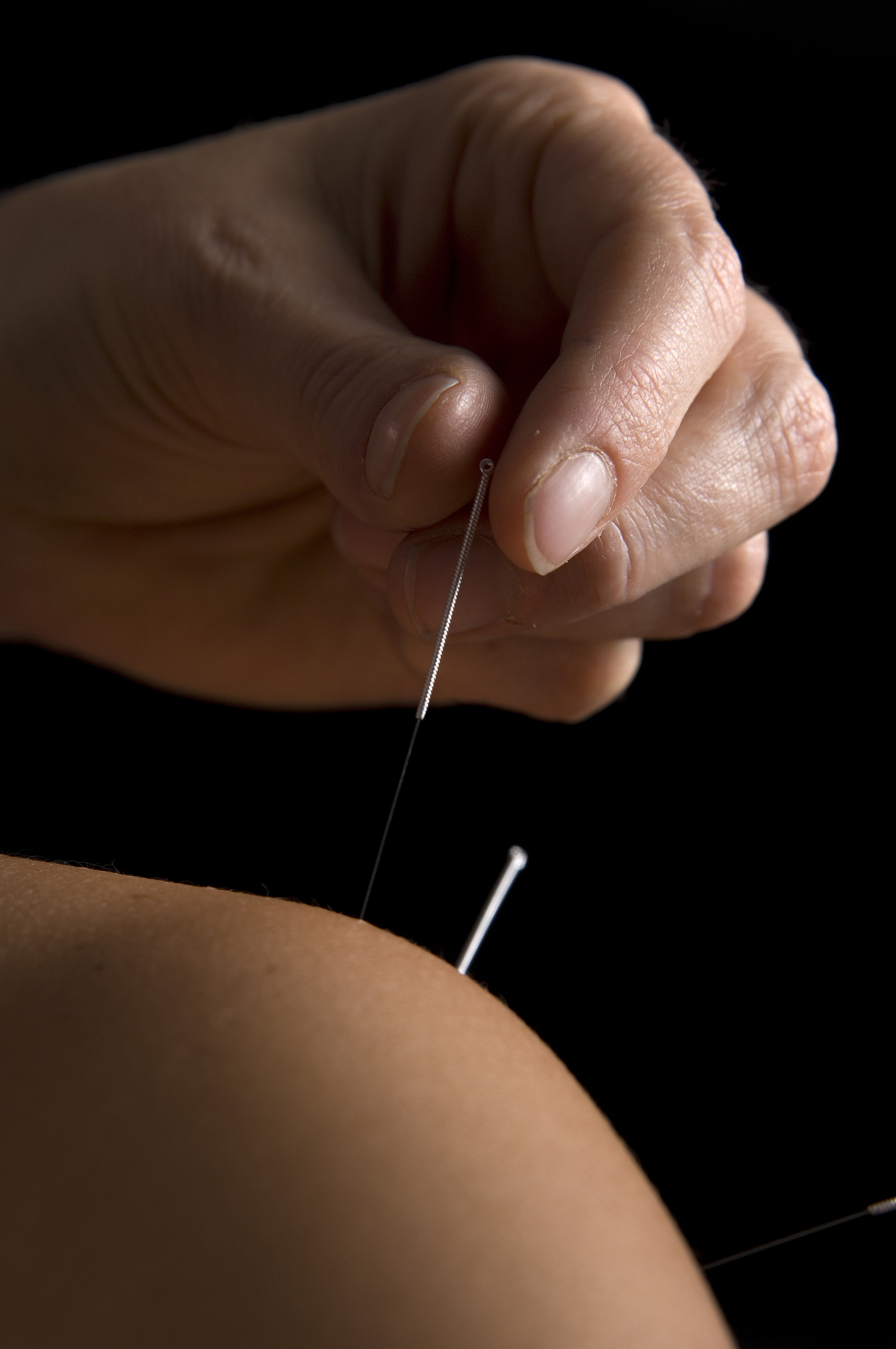
We know from research that acupuncture affects many bodily systems, so here we shall take a look at the nervous system and its chemical messengers: neurotransmitters.
In simple terms, a neurotransmitter is a chemical substance released at the end of a nerve fibre, which diffuses across a synapse (junction between nerves), and transmits the signal along to a nerve fibre or muscle fibre, for example.
This process is involved in the transmission of pain signals in the body, and is also one of the well-understood mechanisms of acupuncture pain relief. The role of acupuncture in modulating neurotransmitters involved in pain has been well discussed, as well as researched in great detail.
Specific neurotransmitters, and acupuncture’s effect on them:
Zhang et al (2022) give the research on those in turn; opioid peptides; γ-Aminobutyric acid (GABA); Norepinephrine; 5-Hydroxytryptamine (5-HT) aka serotonin; and glutamate.
The researchers look in detail about what acupuncture research has shown in terms of mechanisms of action for each neurotransmitter, and to summarise:
- Endogenous opioid peptides (a type of neurotransmitter) are produced in the body as a direct result of acupuncture treatment. These have been shown in numerous studies to have a positive effect on analgesia (pain relief). By name, these are enkephalins, endomorphins, dynorphins, and nociceptin, and they are the body’s own natural painkilling substances
- γ-Aminobutyric acid (GABA); this is an inhibitory neurotransmitter in the central nervous system. It has a painkilling effect. It has been demonstrated through research studies that acupuncture can upregulate GABA expression; another part of how acupuncture helps with pain
- Norepinephrine (noradrenalin in the UK); another neurotransmitter, the release of which is enhanced by acupuncture. Norepinephrine is also capable of inhibiting pain in the body
- 5-Hydroxytryptamine (5-HT), or serotonin; is a neurotransmitter that is involved in analgesia (pain relief). 5-HT is secreted in the brain during acupuncture administration, making it another known mechanism of action for acupuncture analgesia
- Glutamate; a central nervous system neurotransmitter, is involved in the transmission of pain signals in the spinal cord. Acupuncture downregulates glutamate, as part of how it provides pain relief
Overall a combination of demonstratable mechanisms is clearly at play, and can be seen and measured to be the cause of why acupuncture can help pain.
How were the studies done?

Studies on mechanisms of acupuncture analgesia are based on animal models, where levels of neurotransmitters and their effects are measured objectively, removing the possibility of placebo effect as a cause of pain relief.
Human trials are also used where this is measurable in an ethical and objective way, through fMRI (brain scans showing which areas light up), and blood levels of neurotransmitters as well as pain ratings.
A complicated picture
There are other analgesic mechanisms of acupuncture besides those above, and it is hard to unpick the overall contributions of each, and it may be the case that it depends upon the region targeted, quality of pain and other factors. For this reason, the acupuncturist’s experience and overall assessment of the individual on the day of treatment contribute to the overall outcome.
Reference:
Zhang, M., Shi, L., Deng, S., Sang, B., Chen, J., Zhuo, B., Qin, C., Lyu, Y., Liu, C., Zhang, J. and Meng, Z., 2022. Effective oriental magic for analgesia: acupuncture. Evidence-Based Complementary and Alternative Medicine, 2022. https://www.hindawi.com/journals/ecam/2022/1451342/
Bibliography:
Li, S.K., Liao, W.D., Zhao, J. and Cao, X.W., 2020. Effects of acupuncture on plasma endogenous opioid peptides in patients with stroke-associated headache in convalescence. Zhen ci yan jiu= Acupuncture Research, 45(12), pp.995-999.
Lin, J.G., Kotha, P. and Chen, Y.H., 2022. Understandings of acupuncture application and mechanisms. American Journal of Translational Research, 14(3), p.1469.
Petti, F.., Bangrazi, A., Liguori, A., Reale, G. and Ippoliti, F., 1998. Effects of acupuncture on immune response related to opioid-like peptides. Journal of Traditional Chinese Medicine 18(1), pp.55-63.
Trento, M.M.S., Moré, A.O.O., Duarte, E.C.W. and Martins, D.F., 2021. Peripheral receptors and neuromediators involved in the antihyperalgesic effects of acupuncture: a state-of-the-art review. Pflügers Archiv-European Journal of Physiology, 473(4), pp.573-593.
Wang, W.S., Xi, H.Y., Fu, G., Fan, X.Z. and Guo, M., 2022. Study on the Mechanism of Electroacupuncture in the Treatment of Neuropathic Pain Based on Vesicular Glutamate Transporter 2/Toll Like Receptor 4 Signal Pathway. Indian Journal of Pharmaceutical Sciences, pp.31-37.
Wu, W.Z., Zheng, S.Y., Liu, C.Y., Qin, S., Wang, X.Q., Hu, J.L., Wan, Q.Y., Zhao, Y.N. and Xi, H.Q., 2021. Effect of Tongdu Tiaoshen acupuncture on serum GABA and CORT levels in patients with chronic insomnia. Zhongguo Zhen jiu= Chinese Acupuncture & Moxibustion, 41(7), pp.721-724.